
Pfizer kan tjäna 17 miljarder dollar – på Mercks substans
Läkemedelsjätten Pfizer ser ut att kunna tjäna 17 miljarder dollar på sitt nya läkemedel för behandling av covid-19. Men läkemedlet baseras delvis på en upptäckt som konkurrenten Merck har ett patent på, men för en behandling mot hepatit. Att Merck blir omsprungna av en konkurrent med en av bolagets egna nyckelsubstanser adderar till en hård covidresa för läkemedelsjätten. Tillsammans med Sanofi och Glaxosmithkline tillhör Merck de läkemedelsbolag som misslyckats med att ta fram ett användbart covidvaccin och därmed missat vad som bedöms vara en marknad på 85 miljarder dollar årligen, skriver Bloomberg.
Merck’s Covid Pill Fumble Gives Pfizer Potential $17 Billion Win
The drugmaker shelved a 10-year-old drug that’s provided a key component in its rival’s coronavirus treatment.
John Lauerman, Bloomberg Businessweek, 3 February 2022
— With Susan Decker and Cynthia Koons
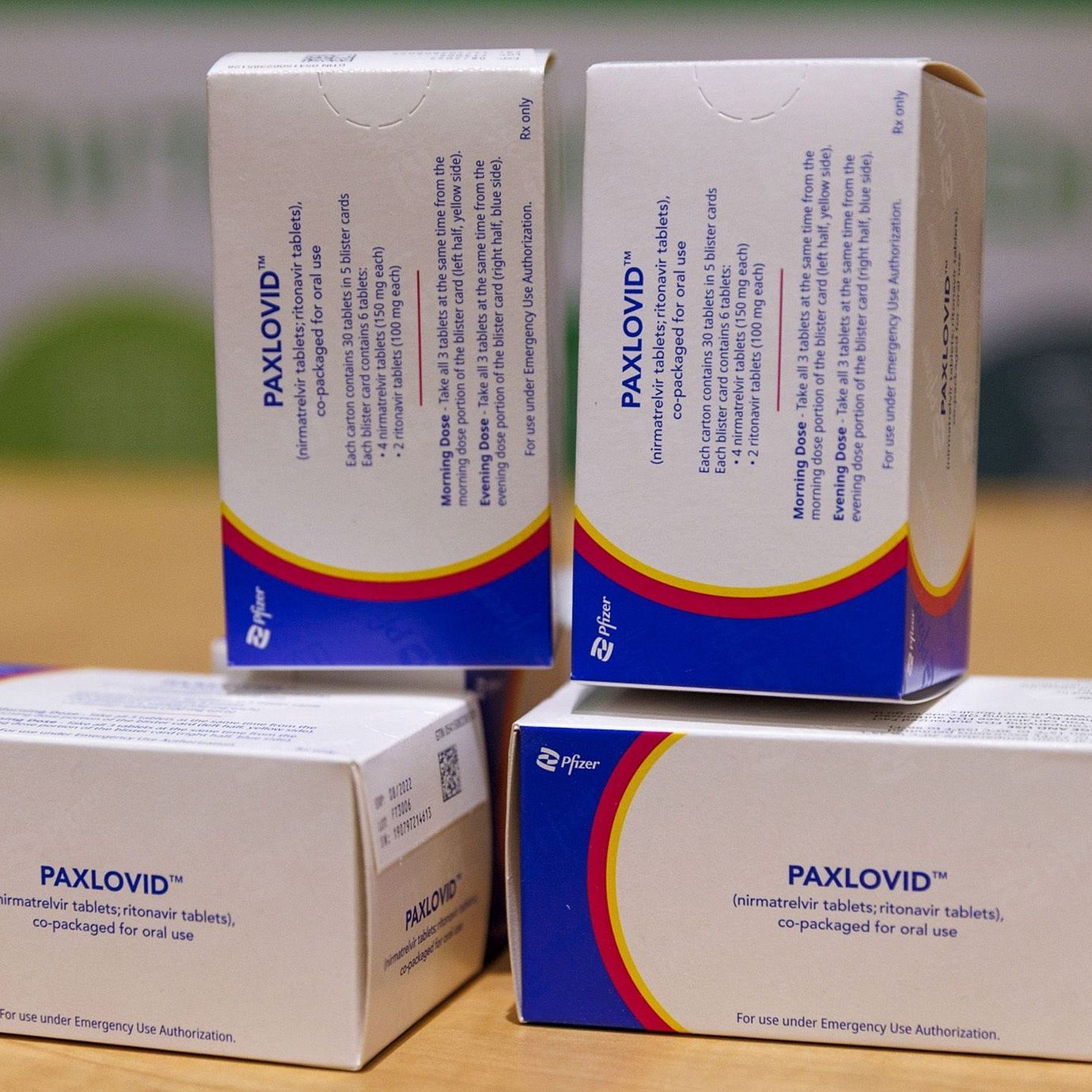
Almost as quickly as Covid-19 erupted in early 2020, so too did the rush to find drugs, either old or new, to treat the contagion spreading around the world. While researchers soon identified some that quelled late-stage symptoms or weakly restrained the virus, Paxlovid, a pill from Pfizer Inc. that prevents severe disease, appears poised to take a solid lead in the lucrative coronavirus treatment market.
Yet an important component of Pfizer’s antiviral has links to a drug from rival Merck: boceprevir, developed decades ago to fight hepatitis C. That fragment accounts for at least 20% of Paxlovid’s coronavirus-fighting power — and perhaps much more — researchers estimate, and a key patent on the larger molecule it comes from still resides with Merck.
Several labs have noted the potential of boceprevir, a protease inhibitor that Merck sold earlier under the brand name Victrelis. But as developers at universities began looking for ways to use it and similar compounds to make Covid drugs over the past two years, Merck sat on the sidelines.
Bypassing the drug while a rival seems set to profit handsomely from one of its key parts adds to Merck’s saga of Covid futility. Along with Sanofi and GlaxoSmithKline Plc, Merck is among the big drugmakers that have still failed to devise a usable coronavirus vaccine in the world’s biggest infectious-disease crisis in a century and partake in a market for Covid shots that health analytics firm Airfinity Ltd. estimates will be worth $85 billion this year.
Pfizer alone forecast $31 billion in 2022 Covid vaccine revenue. It will sop up about $17 billion more in Paxlovid sales this year, while Merck’s Covid pill, based on a different mechanism, molnupiravir, will realize only about $2.5 billion, Airfinity estimates. Merck on Feb. 3 trimmed the upper end of its 2022 forecast of molnupiravir sales to $6 billion, down from its earlier prediction that the drug might log up to $7 billion by yearend.
Merck still holds the key patent portfolio on boceprevir, which is expected to expire in 2024, according to a spokesperson. Early on in the pandemic, company researchers screened its libraries of drug candidates, including boceprevir, which was found not to be sufficiently potent against Covid, the spokesperson said.
The dose of boceprevir needed to achieve an antiviral effect against the coronavirus was estimated to be far greater than the amounts indicated in the drug’s prescribing information, Merck’s spokesperson said, or it would have to be used in combination with other therapies to enhance its potency.
That assessment apparently led Merck to look elsewhere for a coronavirus treatment, while part of the company’s discovery is now incorporated into Pfizer’s potential blockbuster pill.
Merck’s situation isn’t uncommon. Pharmaceutical companies often have millions of experimental compounds available to them, and one of the challenges is to match those molecules with the right disease. Other labs and companies will often spot suitable niches for drugs or their components before their discoverers, says Ashley Brown, a University of Florida expert in antivirals who works on repurposing drugs.
“You see a compound that’s been tested out on a particular virus, and you can buy it and try it out for yourself on something else”
“You see a compound that’s been tested out on a particular virus,” she says, “and you can buy it and try it out for yourself on something else.”
Merck didn’t say why it hasn’t investigated combinations with boceprevir, as Pfizer did, or whether it might enforce its patent on the component. For Paxlovid, a lot depends on how Merck’s patents are written and how they describe the portion echoed in the Pfizer drug, says Michael Carrier, a law professor at Rutgers University. The key question is whether the boceprevir piece “is one that’s protected by Merck or one that isn’t, in which case Pfizer would be free to use it,” he says. The companies could also work out a settlement, which wouldn’t necessarily be disclosed, he says.
A longtime leader in battling infectious disease, Merck looked headed for a Covid comeback through a partnership brokered by Moncef Slaoui, chief scientist for Operation Warp Speed during the Trump administration. Slaoui put Merck together with OncoImmune Inc., a tiny company developing an inflammation-fighter aimed at stopping some of Covid’s worst effects.
Merck paid $425 million in 2020 to take over the company, and the government agreed to pay the drugmaker $356 million for supplies of the experimental medication, called MK-7110. Months later regulators said the compound was unlikely to be cleared on the basis of available data, and Merck halted development, recording a $207 million charge.
“I thought they would jump into it, I was a little surprised”
Since then, Merck’s Covid efforts have focused on development of molnupiravir in partnership with Ridgeback Biotherapeutics LP. The pill fights the virus by inducing genetic flaws in replication, a mechanism that’s raised concerns about sparking drug-resistant Covid variants or causing DNA damage in growing children and fetuses.
Moreover, molnupiravir is only about 30% effective at preventing Covid deaths and hospitalizations among high-risk patients, compared with about 90% efficacy for Paxlovid. Guidelines from the U.S. National Institutes of Health specify that molnupiravir is the last option for outpatient Covid treatment, for use only when other medications — including Paxlovid, Glaxo and Vir Biotechnology Inc.’s sotrovimab, and Gilead Sciences Inc.’s remdesivir — can’t be given.
Hepatitis C and coronaviruses are both RNA viruses that use similar proteases to rip apart proteins to make copies of themselves. Alex Domling, a drug designer at the University of Groningen in the Netherlands, says he first started looking for drugs that could be repurposed to treat SARS-CoV-2 early in the pandemic and filed for a patent on the use of boceprevir to treat Covid a few months into 2020. Separate labs at Rutgers University, Stanford, and the University of Arizona also investigated its anti-Covid activity. But Merck demurred.
“I thought they would jump into it,” says George Njoroge, the Kenya-born scientist who discovered boceprevir. “I was a little surprised.”
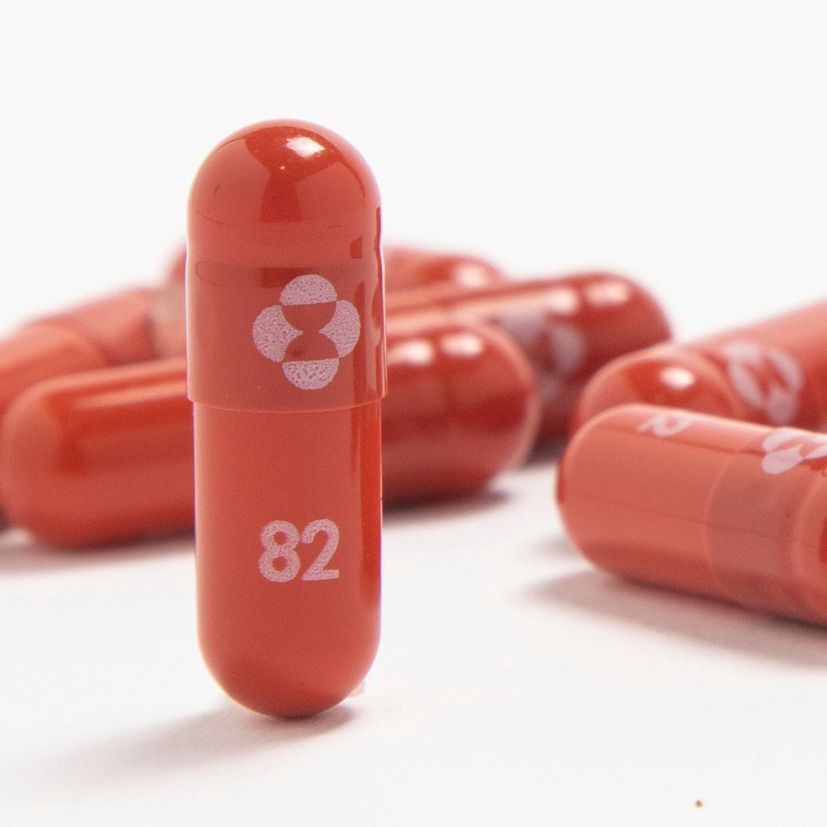
Laboratories around the world continue to look at boceprevir as a possible gateway to the lucrative market for Covid pills, and Domling says the compound still offers potential. “It would be easy to test,” says Domling, who says he’s also looking at other, unrelated molecules. “It would not be too costly, and it would be interesting to see the result.”
Boceprevir’s story began in the mid-1990s when researchers were desperately seeking new therapies for hepatitis C, a potentially deadly infection that was then emerging. Njoroge, 67, was then a scientist at Schering Plough, the drugmaker Merck bought for about $40 billion in 2009. He’d already had some success looking for anticancer drugs, and Schering sent him off in search of a new treatment for the liver disease that was spreading to millions worldwide.
Njoroge decided to look for ways to block the protease. The enzyme is vital to reproduction and, unlike some other viral proteins, doesn’t evolve much; that means inhibitors can retain their power against variants. What Njoroge needed was something that fit into the enzyme, blocking the spot where targeted proteins normally adhere. He carefully examined how the protease interlocks with proteins in human cells and found that substituting a key piece in an experimental inhibitor helped the biological puzzle pieces come together.
The substitute piece, a modified ring structure including the amino acid proline, improved the drug’s stability, preventing it from being easily broken down, and allowed it to be used in a smaller form. It was the key Njoroge was looking for.
“You do the heavy lifting and have to publish how you did it, so you pave the road for everyone”
“It raised the potency, made the molecule drug-like, and gave it a molecular weight that could get into cells and still have pharmacokinetic activity,” says Njoroge, who has since retired and is establishing an institute outside Nairobi to train aspiring African drug scientists. “I said, ‘We have a drug.’”
The approach won Njoroge a slew of scientific accolades, including being named a 2012 Hero of Chemistry by the American Chemical Society. But after Victrelis made its debut, rivals piled into hepatitis C treatment, devising powerful blockbusters such as Gilead’s Harvoni. Victrelis sales peaked in 2012 at about $500 million, and Merck pulled it from the market in 2015. “You do the heavy lifting and have to publish how you did it, so you pave the road for everyone,” Njoroge says.
Then came Covid. Pfizer had a different protease inhibitor on hand that it already knew targeted coronaviruses, says Brown, the University of Florida researcher. But Merck would have had to do a lot more work on boceprevir to make a Covid pill, she says. “Pfizer wasn’t starting from boceprevir,” she says. “They had something that bound and inhibited the active site” on the viral enzyme.
Paxlovid was the product of a drug discovery process that began in 2020, Pfizer said in a statement. Structures in the drug that resemble those in Merck’s combine with other components to create a drug that is “hundreds of fold more potent than boceprevir,” Pfizer said.

To Stanford drug researcher Michael Lin, who says he’s read all of Njoroge’s papers, the boceprevir pioneer is a scientific hero and deserves some credit. The proline ring was a critical innovation, he says, because it made the drug far less reactive with cells and tissues such as the gut. That’s what allowed boceprevir — and now allows Paxlovid — to be used as an oral pill, rather than an infusion, he says.
Pfizer did important, significant work to make Paxlovid, but they haven’t sufficiently acknowledged the contribution of boceprevir, Lin says. “For them to say it’s all internal and there were no external ideas is just intellectually highly unlikely.” The proline ring is “copied verbatim from boceprevir,” he says. “Who are they kidding?”
For more articles like this please visit us at bloomberg.com.